IVF Success Rates by Age: Realistic Expectations Based on Current Data
IVF success rates by age explained with current SART and HFEA data — live birth rates per cycle at every age, what affects your odds, and how to have an honest conversation with your clinic.
Probar herramientas relacionadas
Use nuestras calculadoras revisadas médicamente para obtener información precisa.
Table of Contents
- The Most Important Number: Live Birth Rate Per Cycle Started
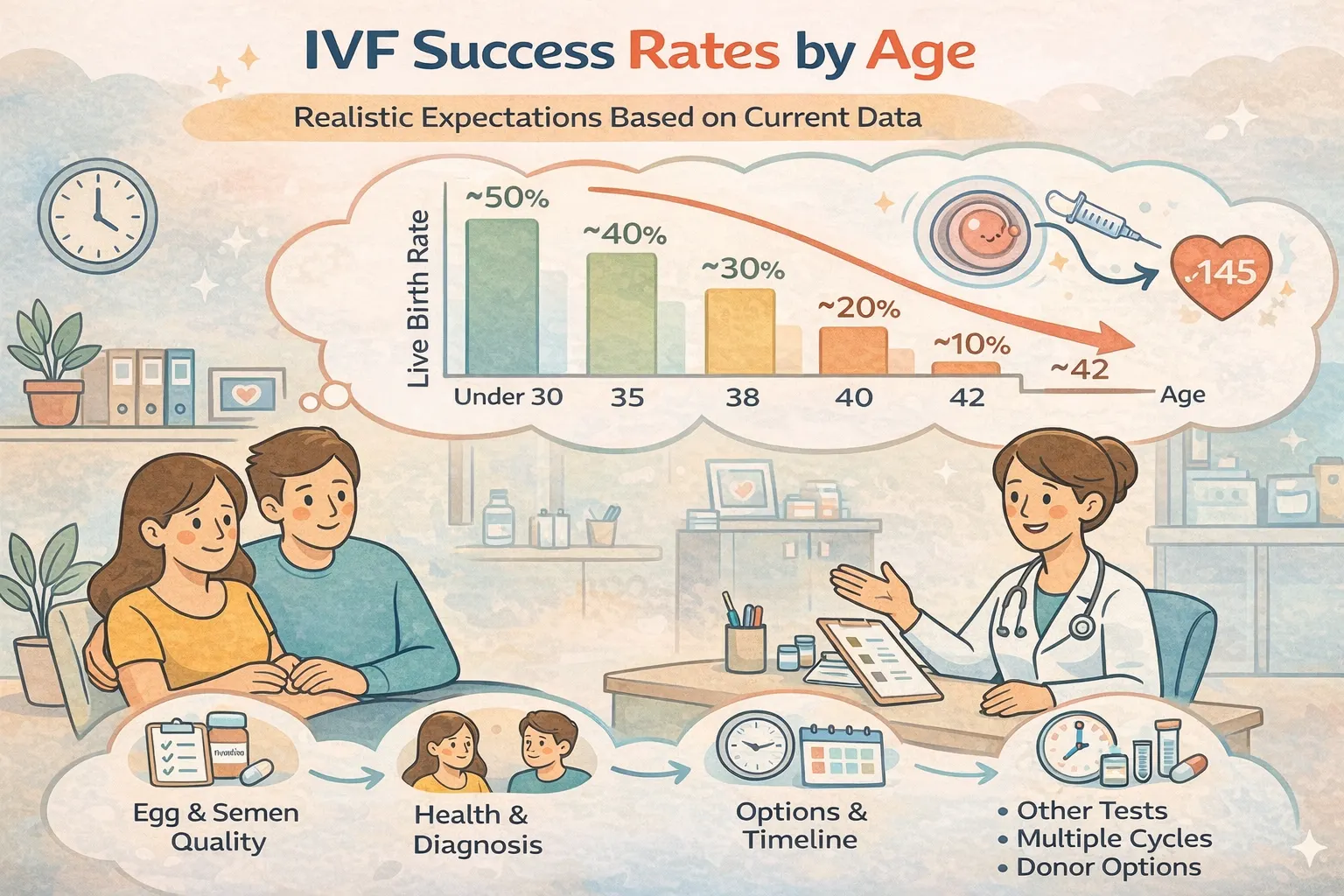
- IVF Live Birth Rates by Age: Current Data
- Cumulative Live Birth Rates: The Bigger Picture
- Factors That Affect IVF Success Rates Beyond Age
- Questions to Ask Your Clinic Before Committing
- The Emotional Reality of IVF: Managing Expectations
- Frequently Asked Questions (FAQ)
- References and Further Reading
The Most Important Number: Live Birth Rate Per Cycle Started
Before examining age-specific data, understanding which statistic to focus on is critical.
Why "Pregnancy Rate" Is Misleading
Most IVF clinics historically reported clinical pregnancy rates — the proportion of cycles in which a fetal heartbeat was detected on ultrasound at 6–7 weeks. This number is significantly higher than the live birth rate because it does not account for:
- Early pregnancy losses (miscarriages, which are significantly more common with IVF, particularly in older women)
- Late pregnancy complications
- Cycles that were cancelled before embryo transfer (due to poor response, no fertilisation, or no surviving embryos)
A clinic reporting a 55% clinical pregnancy rate may have a 40% live birth rate — or less.
The Number You Should Ask For
Live birth rate per cycle started — also called the live delivery rate per intended egg retrieval in current SART reporting.
This is the most conservative and most honest measure: the number of women who started a fresh IVF cycle (took injections, had a retrieval attempt) and ultimately took a living baby home, divided by the total number of cycles started.
Always ask your clinic: "What is your live birth rate per cycle started, stratified by patient age?"
IVF Live Birth Rates by Age: Current Data
The following data is drawn from the most recently available SART (Society for Assisted Reproductive Technology) and HFEA (Human Fertilisation and Embryology Authority) published national outcomes reports. These are national averages — your individual clinic's results may differ.
Using Own Eggs (Fresh Cycles)
| Age Group | Live Birth Rate Per Cycle Started |
|---|---|
| Under 35 | 40–48% |
| 35–37 | 31–38% |
| 38–40 | 20–26% |
| 41–42 | 11–15% |
| 43–44 | 5–7% |
| Over 44 | 2–4% |
Using Own Eggs (Frozen Embryo Transfer — FET)
Frozen embryo transfer cycles using embryos from a previous retrieval have become the dominant approach in many clinics, offering:
- The ability to biopsy embryos for preimplantation genetic testing (PGT-A)
- A more receptive endometrial environment (avoiding ovarian hyperstimulation)
- Flexibility in timing
| Age at Egg Retrieval (FET using own embryos) | Live Birth Rate Per Transfer |
|---|---|
| Under 35 | 45–52% |
| 35–37 | 36–43% |
| 38–40 | 26–33% |
| 41–42 | 15–20% |
| 43–44 | 8–12% |
Why FET rates are often higher than fresh: The endometrium is better prepared in a frozen cycle — the hormonal environment of the transfer cycle is controlled, and ovarian hyperstimulation is absent. This improves implantation rates.
Using Donor Eggs
When donor eggs are used, the live birth rate is primarily determined by the donor's age (typically under 35 in most donor programmes) rather than the recipient's age. Recipient age has a relatively modest additional effect.
| Recipient Age | Live Birth Rate Per Transfer (Donor Eggs) |
|---|---|
| Under 40 | 47–55% |
| 40–44 | 43–52% |
| 45–49 | 38–48% |
| 50+ | 30–42% |
The relative consistency of donor egg success rates across recipient ages demonstrates clearly that the declining success of IVF in older women using their own eggs is primarily a function of egg quality, not uterine receptivity.
"This is one of the most important clinical insights I share with patients over 40 considering treatment options," says Dr. Preeti Agarwal. "The uterus does not age as rapidly as the eggs. A 44-year-old woman's uterus can successfully carry a donor egg pregnancy — it is the eggs that carry the most significant age-related risk. This is not a reason to rush to donor eggs, but it is important context for discussing realistic options."
Cumulative Live Birth Rates: The Bigger Picture
The figures above represent a single cycle. Most patients who achieve a live birth from IVF do so over multiple cycles, and cumulative success rates are significantly more encouraging than per-cycle rates.
HFEA data shows that after up to 6 cycles of IVF using own eggs:
| Age | Cumulative Live Birth Rate (Up to 6 Cycles) |
|---|---|
| Under 35 | 79–85% |
| 35–37 | 63–72% |
| 38–39 | 46–55% |
| 40–42 | 27–35% |
| 43–44 | 14–20% |
These cumulative figures include both fresh and frozen embryo transfers from all retrievals and better represent the true likelihood of success for patients who are able to continue treatment.
Important caveats:
- These figures represent patients who completed multiple cycles — those who stopped treatment due to cost, emotional burden, or poor prognosis are not included in cycle 4–6 data, which introduces selection bias
- Not everyone produces viable embryos for multiple cycles, particularly at older ages
- Some patients achieve success on the first cycle; others do not after six
Factors That Affect IVF Success Rates Beyond Age
Age is the single most predictive factor for IVF success, but it is not the only one. These factors significantly modify outcome:
Ovarian Reserve
Assessed by Anti-Müllerian Hormone (AMH) and antral follicle count (AFC), ovarian reserve measures the quantity of remaining eggs. Low ovarian reserve at any age is associated with reduced egg retrieval numbers, fewer viable embryos, and lower live birth rates.
However, ovarian reserve tests measure quantity, not quality. Some women with low AMH produce few but excellent-quality eggs; others with higher AMH have eggs of poor quality. Reserve tests help predict response to stimulation but are imperfect predictors of outcome.
If you want to understand your own ovarian reserve picture, our AMH Level Predictor interprets AMH results in context of your age.
Cause of Infertility
- Tubal factor infertility: IVF bypasses the tubes entirely; outcomes are generally good
- Male factor infertility: With ICSI (intracytoplasmic sperm injection), even severe male factor can be overcome if retrievable sperm are available
- Unexplained infertility: Outcomes broadly follow age-based norms
- Diminished ovarian reserve: Success rates below age-average norms
- Endometriosis: Mildly to moderately reduced success rates, though this varies significantly by stage and whether surgery has been performed
- Uterine abnormalities: Fibroids (depending on position), polyps, and structural anomalies reduce implantation success and should be corrected before treatment where possible
Embryo Quality and PGT-A
Preimplantation genetic testing for aneuploidy (PGT-A) — chromosome screening of biopsied embryos before transfer — identifies euploid (chromosomally normal) embryos for transfer.
Benefits:
- Significantly reduces miscarriage risk (particularly relevant for women over 38 where aneuploidy rates are high)
- Increases the per-transfer live birth rate by selecting only viable embryos
- Reduces time to live birth by avoiding failed transfers with aneuploid embryos
Limitations:
- Adds cost
- Some patients have no euploid embryos to transfer (particularly common over 40)
- Not universally recommended — benefit is clearest in women over 38 and those with recurrent implantation failure
Clinic Experience and Laboratory Quality
IVF outcomes are significantly influenced by clinic and laboratory quality — embryology laboratory standards, stimulation protocol expertise, and culture media. National data shows meaningful variation between clinics that cannot be explained solely by patient demographics. When choosing a clinic, look at age-stratified live birth rates rather than unadjusted headline rates.
Lifestyle Factors
- Smoking: Reduces ovarian response to stimulation and reduces live birth rates by 20–30%
- BMI: Obesity is associated with reduced ovarian response, higher cancellation rates, reduced implantation, and higher miscarriage rates. BMI over 30 significantly reduces success.
- Alcohol: Regular alcohol consumption is associated with reduced IVF success; abstaining during treatment is recommended
- Stress: While stress does not "cause" IVF failure, evidence suggests that mindfulness-based stress reduction during treatment may modestly improve outcomes — and significantly improves wellbeing during what is an intensely stressful process
Questions to Ask Your Clinic Before Committing
Armed with this understanding, here are the specific questions every patient should ask:
- What is your live birth rate per cycle started, for my age group, using my own eggs?
- What is your live birth rate for frozen embryo transfers for my age group?
- How many egg retrievals do I typically need to accumulate enough embryos for transfer?
- What proportion of patients in my age group have no viable embryos to transfer?
- Do you recommend PGT-A for my situation, and what does the data show for your laboratory?
- What is the total estimated cost including monitoring, medications, and genetic testing if applicable?
- What is your cancellation rate at egg retrieval — the proportion of cycles cancelled before retrieval?
A clinic that answers these questions clearly and honestly — without redirecting you to more favourable statistics — is demonstrating the transparency that quality care requires.
The Emotional Reality of IVF: Managing Expectations
Numbers are essential — but they do not capture the full picture of what IVF involves.
Each cycle carries a significant emotional investment. A failed cycle is genuinely a loss — not in the clinical sense, but in the sense that hope has been built and then withdrawn. Recalibrating after a failed cycle, particularly a second or third, is psychologically demanding in ways that are difficult to anticipate.
Evidence-based support during IVF:
- Psychological counselling with an IVF-experienced therapist is strongly recommended before and during treatment at any reputable clinic
- Partner communication — couples who discuss their mutual limits (number of cycles, use of donor eggs, stopping criteria) before beginning treatment report significantly lower conflict and better outcomes regardless of IVF result
- Mindfulness and stress management — not because stress causes failure, but because the process is easier to navigate from a position of psychological stability
- Support communities — peer support from others going through IVF can normalise the emotional experience in ways professional support cannot fully replicate
Frequently Asked Questions (FAQ)
Q: What is the average IVF success rate? A: There is no single meaningful "average" — success rates vary enormously by age. For women under 35 using their own eggs, live birth rates per cycle started are approximately 40–48% at experienced clinics. For women over 43 using their own eggs, the rate falls to 2–7%. Any IVF statistic quoted without age stratification is not useful.
Q: How many IVF cycles does it take on average to get pregnant? A: Most women who ultimately succeed do so within 3 cycles. HFEA cumulative data shows that success rates continue to rise with each additional cycle through cycle 6, though the incremental gain per cycle decreases beyond cycle 3. For women under 38, approximately 50–60% succeed within 3 cycles. For women over 40, more cycles may be needed, and donor egg discussion often becomes relevant after 2–3 unsuccessful own-egg cycles.
Q: Does IVF success rate decrease after a failed cycle? A: No — a prior failed cycle does not reduce your statistical chances in the next cycle, provided your situation has not changed and stimulation was optimised. For most age groups, the per-cycle probability remains approximately stable across the first 3–4 cycles. Some evidence suggests a slight improvement in outcomes in cycle 2–3 as protocols are refined.
Q: At what age should I consider switching to donor eggs? A: This is a deeply personal decision with no universal threshold. Clinically, donor eggs become worth discussing when own-egg cycles consistently yield few or no euploid embryos, when AMH and AFC are very low, or when 2–3 own-egg cycles have failed. For women over 43, the likelihood of live birth with own eggs is below 10% per cycle, and the cumulative success over multiple cycles remains modest. Many women have a strong preference to try own eggs first regardless of statistics — this is valid and should be respected in shared decision-making with a reproductive specialist.
Q: Is IVF less successful for women with PCOS? A: Women with PCOS typically produce more eggs in response to stimulation and have normal to above-normal live birth rates from IVF. The main concern in PCOS is ovarian hyperstimulation syndrome (OHSS) — the risk of which is managed by careful protocol choice (lower doses, GnRH antagonist protocols, freeze-all strategies with FET). Overall, women with PCOS do well with IVF when protocols are appropriately chosen.
Q: What percentage of IVF cycles are cancelled before egg retrieval? A: National cancellation rates before retrieval average approximately 12–15% across all age groups. The most common reasons are poor ovarian response (too few follicles developing), over-response with OHSS risk, or failure of follicle maturation. Cancellation rates are higher in older women and those with low ovarian reserve.
Q: Can lifestyle changes improve my IVF success rate? A: Yes. Stopping smoking, achieving a healthy BMI, abstaining from alcohol, optimising vitamin D levels, and taking appropriate supplements (CoQ10, DHEA in some protocols) are associated with modest but real improvements in IVF outcomes. These changes take approximately 3 months to fully impact egg quality (one full spermatogenesis and folliculogenesis cycle). Beginning these changes before your first cycle is worthwhile.
Q: What is the difference between IVF and ICSI? A: In standard IVF, eggs and sperm are combined in a dish and fertilisation occurs naturally. In ICSI (intracytoplasmic sperm injection), a single sperm is injected directly into each egg — used when male factor infertility is present, when previous IVF cycles showed poor fertilisation, or increasingly as a default approach at many clinics. ICSI does not significantly improve live birth rates over conventional IVF when sperm parameters are normal.
References and Further Reading
-
HFEA — Fertility Treatment Trends and Figures:
https://www.hfea.gov.uk/about-us/publications/research-and-data -
ACOG — Assisted Reproductive Technology:
https://www.acog.org/clinical/clinical-guidance/committee-opinion/articles/2016/09/perinatal-risks-associated-with-assisted-reproductive-technology -
ASRM — IVF Success Rates:
https://www.reproductivefacts.org/news-and-publications/patient-fact-sheets-and-booklets -
CDC — ART Success Rates:
https://www.cdc.gov/art/success-rates/ -
NICE Guideline CG156 — Fertility: Assessment and Treatment:
https://www.nice.org.uk/guidance/cg156
Medical Disclaimer
This article is for informational and educational purposes only. It does not constitute medical advice, diagnosis, or treatment. IVF success rates presented are national averages and individual outcomes vary significantly based on personal medical history, ovarian reserve, cause of infertility, and clinic-specific factors. Always discuss your individual prognosis with a qualified reproductive endocrinologist or fertility specialist before making decisions about treatment. The emotional and financial demands of IVF are significant — psychological support throughout the process is strongly encouraged.
About the Author
Abhilasha Mishra is a health and wellness writer specializing in fertility, assisted reproduction, and reproductive medicine. She writes to ensure that those navigating complex fertility decisions have access to accurate, honestly communicated clinical information.